I Can Spell Electroencephalogram (EEG)
Recently, my neurologist ordered an EEG test for my epilepsy. EEG stands for electroencephalogram. An EEG records the electrical activity in your brain and it helps doctors detect abnormal electrical activity of the brain. Most types of EEG tests are considered relatively painless. However, like any medical test, from scheduling to prepping for the test, an EEG can always include some inconveniences and annoyances. Anyone who has ever had to remove EEG glue from their hair, understands why I call an EEG “relatively” painless.
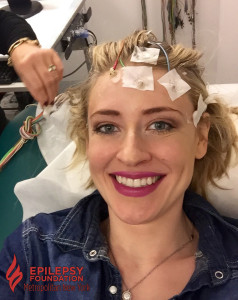
I had my first EEG test shortly after I was originally diagnosed with epilepsy when I was six years old. When my parents told me I had to undergo a new test related to my epilepsy, my first question was: “Are there any needles involved?” Luckily, my parents reassured me I would not be receiving a shot, getting an I.V. drip, or giving any blood. Plus, since my doctor prescribed me a sleep deprived EEG, the test prep required me to stay up late, preferably all night. Also, I got to miss a day of school, which was pretty cool! The next morning, my mother took me to my neurologist’s EEG lab. I was placed on a hospital bed and the technician glued electrodes to my head. After an hour of the technician asking me to breathe deeply and blink my eyes, they let me fall asleep. After I woke up, my electrodes were being removed from my head, and I returned home to go to bed. After several sleep deprived EEGs, I realized my mom also had to stay awake all night with me and miss work the next day. While I got to fall asleep for four hours during my EEG, my mom remained awake speaking with the technician or doctor. Now, as an adult, I understand how much an epilepsy diagnosis affects the entire family, from diagnosis to treatment.
In my twenties, I underwent a medication change because I began having a lot of seizures, again. My neurologist prescribed me several 72 hour ambulatory EEGs. For three days, I had a head full of glued-on electrodes. The electrodes were connected to wires, and the wires were connected to a small box recording the results. I could go anywhere, as long as I was still connected to my EEG box and electrodes. At work, I hid my electrode-covered head with a stylish beanie or scarf, allowing me to feel “normal.” Unfortunately, by the end of the first 48 hours, my head was itching like crazy. There was no beanie or scarf to alleviate my itchy head without removing the electrodes; but if these were to fall off, the EEG may have to be repeated! Finally, after the 72 hours, I would return to my neurologist’s office to have the electrodes removed.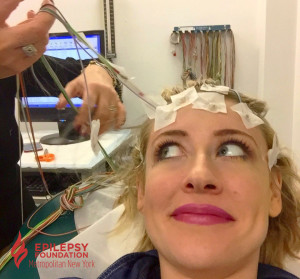
After any EEG, the inevitable issue of how to remove EEG glue arises. During this period of my life, I was not connected with the Epilepsy Foundation of Metropolitan New York, so I did not know the Epilepsy Foundation’s magic trick for removing EEG glue:
· Add 5 to 7 crushed aspirin to half a cup of hot water to dissolve. Then, add 2 good size squirts of shampoo, 4 tablespoons witch hazel or seabreeze, and mix well together. Massage the mixture through wet hair and let it sit for about 15 to 20 minutes. Finally, begin to comb through your hair after an allotted time has passed. Rinse and use shampoo and conditioner as usual.
I have never had to undergo a video-telemetry EEG test, which requires a patient to spend days in a hospital wearing an ambulatory EEG box, while being recorded by a video camera. Additionally, during a video-telemetry EEG test, epilepsy medications may be reduced or withdrawn, to increase the chances that you will have a seizure that can be recorded. So, while there are rarely needles involved, I would not dare to categorize all EEGs as “painless.”
 My recent standard EEG lasted for one hour and took place at my doctor’s office. It was the easiest EEG I had ever experienced. But, like epilepsy, even the types of EEG tests can vary. Like any medical procedure, it is important to stay informed and well prepared for an EEG test. The information an EEG test provides is essential for doctors treating epilepsy. Thankfully, this past EEG was totally painless because I finally knew how to remove EEG glue from my hair!
My recent standard EEG lasted for one hour and took place at my doctor’s office. It was the easiest EEG I had ever experienced. But, like epilepsy, even the types of EEG tests can vary. Like any medical procedure, it is important to stay informed and well prepared for an EEG test. The information an EEG test provides is essential for doctors treating epilepsy. Thankfully, this past EEG was totally painless because I finally knew how to remove EEG glue from my hair!
Prognosis in Infantile Spasms – #EpilepsyNYC Infantile Spasms Awareness Week
Summary:
– The overall intellectual and neurodevelopmental outcome in children with infantile spasms is generally poor
– The long-term prognosis is directly related to the underlying cause of the seizures
– Better developmental outcomes are noted in patients without an identified cause (cryptogenic/idiopathic)
– Although the spasms tend to resolve by early to mid childhood, a majority of the children develop other types of seizures and epilepsies.
– There is a better outcome noted in those patients treated earlier in the course of their seizures, and in those that have an early and sustained response to treatment.

Infantile Spasms
The long-term prognosis of patients with infantile spasms has been studied extensively over the years. Many studies have examined the outcome of infantile spasms including neurodevelopmental and intellectual disabilities, prognostic significance of the EEG, and the development of chronic epilepsy.
The consensus of all of these studies is that the overall outcome, with regards to chronic epilepsy and neurodevelopmental disability is generally poor in patients with infantile spasms.
Chronic Epilepsy
Epileptic spasms usually resolve, latest by mid-childhood, in the majority of patients. Infrequently, spasms may persist in adulthood. Even if the spasms resolve, it has been found that 50-70% of the patients will develop other seizure types. Approximately 50% of the patients with a history of infantile spasms go on to develop chronic intractable epilepsy. There is a strong relationship seen between a history of infantile spasms (IS) and development of Lennox- Gastaut syndrome, with 18-50% of IS patients developing Lennox-Gastaut syndrome.
EEG
While features of hypsarrhythmia define the EEG of patients with infantile spasms, evidence of this abnormality on the first EEG was seen not to influence the response to treatment. However, if the hypsarrhythmia persisted despite treatment, or was atypical and/or asymmetrical, this was seen to adversely influence the long-term outcome.
Neurodevelopmental disability
The most important factor in predicting the cognitive and developmental outcome of patients is etiology.
Mental retardation occurs in about 70 % of patients with infantile spasms, usually involving severe to profound retardation and often associated with other psychiatric problems. Other neurological deficits, such as cerebral palsy, may be seen in about 30-50% of patients.
Most children with infantile spasms experience slowing, plateauing, or regression of their developmental progress.
Studies have consistently shown that infants with symptomatic infantile spasms are at much higher risk (86-90%) of developing mental retardation, autism and other behavioral and cognitive disabilities, compared to infants with idiopathic infantile spasms. Symptomatic infantile spasms, in particular, are associated with autism spectrum disorders (ASD) in up to 35% of cases.
10-20% of patients with normal development prior to the start of their spasms will have normal mental function or only be mildly impaired long-term. 28-50% of patients with idiopathic infantile spasms will go on to have normal or borderline cognitive development.
Mortality
The premature death rate for infantile spasm ranges from 5-31%. Most of the deaths (61%) occurred at or before age 3 years, while only 10% occurred after age 20 years.
In most cases, the mortality is seen to be a result of the underlying neurological cause of the infantile spasms.
Factors for a favorable outcome in Infantile Spasms
• Cryptogenic or idiopathic cause
• Age of onset of spasms > 4 months
• No atypical or partial seizures
• Typical EEG abnormalities – hypsarrhythmia
• Early onset of treatment
• Early and good response to treatment
Treating Infantile Spasms – #EpilepsyNYC Infantile Spasms Awareness Week
Infantile spasms is a potentially devastating early-onset epilepsy that affects infants, typically between three and nine months of age. Many cases of infantile spasms occur in children who are already have brain abnormalities, such as children with tuberous sclerosis, down syndrome, or brain injuries sustained as newborns. However, in about one third of affected infants, infantile spasms occur for no known reason.
There are three first-line treatments used for infantile spasms. Most pediatric neurologists select one of these three as the initial treatment.

First, adrenocorticotropic hormone (ACTH) is a naturally occurring hormone that is made by the pituitary gland. It stimulates the body to produce steroids. There are several versions of ACTH available throughout the world — in the US, physicians can prescribe a pharmaceutical grade purified ACTH for infantile spasms. ACTH must be given by injection into the infant’s thigh twice a day for two weeks, and then gradually tapered over the next several weeks. There are significant side effects. Many babies become very irritable when taking this medication. It increases their appetite, and some gain weight during treatment. ACTH can also increase blood pressure and, on occasion, lead to an increase in the size of the heart. These side effects fade after the medication is stopped.
Second, oral prednisolone is a corticosteroid, which comes as a liquid. This is the same medicine given for children with asthma attacks; although, for infantile spasms we use a higher dose for a longer period of time (usually several weeks). It can have the same side effects as ACTH, but these are usually less severe.
Third, vigabatrin is a medication that comes as a packet of powder, which can be disolved in water. The major worrisome side effect of vigabatrin is loss of peripheral vision. This is uncommon. Usually when vigabatrin is prescribed, the infant will also need to see an ophthalmologist to monitor for this potential side effect.
Current evidence suggests that ACTH has the best overall response rate. The one exception is that for children who have infantile spasms due to tuberous sclerosis, vigabatrin seems to work better.
First-line therapy works between half and three quarters of the time. If it fails, there is not good evidence to guide us on what to try next. Many physicians will switch to a different first-line agent. For example, if a child continues to have seizures after ACTH, the physician may try vigabatrin next. Rarely, a deficiency of vitamin B6 can cause infantile spasms, and many physicians will give infants this vitamin. Other physicians may try dietary therapy. For example, there is a diet called “the ketogenic diet” that avoids carbohydrates and sugars. This diet can lead to changes in how the brain makes fuel for itself, which can, in turn, reduce seizures.
In some cases, children with infantile spasms may have a subtle area of the brain which is abnormal, which is difficult to see on MRI scans. Some physicians will order other kinds of brain scans, such as a PET scan (positron emision tomography), in order to look for these kinds of abnormalities. This is important, because some infants benefit from epilepsy surgery to remove the abnormal area of brain.
Dr. Zachary Grinspan, MD
Weill Cornell
Community Spotlight: Epilepsy Road Warriors Take on the NYC Marathon
From all of us at EFMNY: Our thoughts are with everyone who is recovering from Hurricane Sandy. Currently, our servers are down and our power is out. You can still access our site. However, our staff are unable to access email. We hope to be up and running as soon as possible.
National Epilepsy Awareness Month in Metro New York
As November, National Epilepsy Awareness Month, approaches, we wanted to share some of the ways in which our community is coming together to raise awareness and fund epilepsy education and empowerment programs. You may have read our last post about Team Gabriella and our 1st Annual Into the Light Walk for Epilepsy Awareness on Saturday, November 10th in Hudson River Park (NYC). We’re also excited to introduce you to the Epilepsy Road Warriors, our first team to run the NYC Marathon this Sunday, November 4th. Here are the opening paragraphs of their personal stories. To read their full stories and to learn more about how you can support the team, please visit our team page by clicking HERE or by clicking on each team member’s name below:
The call came early one morning two years ago. My brother, sister-in-law and four year old niece, Siena, were at the hospital. Siena had a grand mal seizure the night before. Paramedics were called and struggled for over 45 minutes to stabilize her. We were stunned. There was no indication prior to this day that she had Epilepsy. There was no family history. This caught us all by surprise.
I was diagnosed with complex partial epilepsy 16 years ago. Regardless of all the ups and downs along the way, I still consider myself to be very fortunate that my condition is very well controlled with medication. To me, no one is perfectly healthy (really); my brain just likes to tease me with unusual signals once in a while, which leads to a seizure. But with such great support from amazing people in my life, nowadays when it happens I have learned to stop asking what I did wrong to deserve this (okay, I usually bitch about it a little bit), get up and move on.
Jennifer Cunningham, Co-Captain:
As a physician – I always thought I understood Epilepsy. I understood the different seizure types. I understood the medications and their side effects. What I didn’t understand was the impact that Epilepsy has on those that suffer from it. That changed when my beautiful and healthy daughter, Nora, suffered her first grand mal seizure at the age of 5. My life and views on everything changed that day.
I first joined New York’s epilepsy community as a professional in 2004. In that capacity, I had the opportunity to work with hundreds of individuals and families affected by seizure disorder. I also became close friends with a co-worker whose father was diagnosed with epilepsy when she was six-years-old. Together, we share a commitment to raise epilepsy awareness, so that people affected by seizures have access to the best treatments, services and quality of life possible.
First, let me explain the grainy photos. They were taken in May, 1981. That’s me and my father running a 10k when he was 33 and I was 6. His favorite moment was when I bent down and kissed the 4 mile marker. A few months after the race, I woke up one morning to find my father convulsing on the floor. I didn’t know that he had had seizures as a teenager, seizures that were vitually ignored at a time when people didn’t want their families associated with epilepsy. I woke my 10-year-old sister and we called our neighbors.
I had my first epileptic seizure when I was seventeen years old. Up until that point, I had never really had any kind of health issue whatsoever. I suddenly went from being able to do basically anything I wanted to being worried about being able to drive, being left alone or even something as mundane as taking a shower. My family was worried sick, and really had no idea as to where to turn or what to expect.
On December 9, 2011 the world was granted an angel, my cousin Mary Kate Szokoli. She was 30 years old and lost to her battle with epilepsy. I am running in the NYC marathon on November 4 in honor of her. I have set a goal of raising $2,500 for the Epilepsy Foundation so that others my become aware of the impacts and educated on living with Epilepsy.
Heres our story I was 13yrs old when I was diagnosed with epilepsy and have been living with it ever since. I am very happy to say that I have been seziure free for 2yrs now. Great right? Well a couple of years ago my little 9yr old sister was diagnosed with epilepsy it crushed my heart I always thought better me then my sisters to have to live with this. Then our other sister had a great idea and started a team called C & E Warriors to encourgae us to walk for the cause on November 10 and to honor her sisters that have to live with this disorder.
Community Spotlight: Walk with Team Gabriella
UP NEXT: THE EPILEPSY ROAD WARRIORS TAKE ON THE NYC MARATHON
 At the Epilepsy Foundation of Metropolitan New York, we have the opportunity to work with the metro area’s leading health providers and advocates as well as extraordinary individuals and families affected by epilepsy. That’s why we’re excited to introduce the first in our Community Spotlight series. This series will highlight the exciting efforts being made within our community each day to increase epilepsy awareness, education and empowerment. This first edition features the story of Team Gabriella as told by her mother, Karen Mendez.
At the Epilepsy Foundation of Metropolitan New York, we have the opportunity to work with the metro area’s leading health providers and advocates as well as extraordinary individuals and families affected by epilepsy. That’s why we’re excited to introduce the first in our Community Spotlight series. This series will highlight the exciting efforts being made within our community each day to increase epilepsy awareness, education and empowerment. This first edition features the story of Team Gabriella as told by her mother, Karen Mendez.
To join Team Gabriella and EFMNY for the 1st Annual Into the Light Walk for Epilepsy Awareness on Saturday, November 10th in Hudson River Park, visit www.epilepsyintothelight.org. For more information, email tpowers@efmny.org or call 212-677-8550.
Gabriella’s Story by Karen Mendez
On December 27, 2007 God blessed me with a beautiful baby girl who I named Gabriella Ashley Mendez. At the age of 2, Gabriella would have these violent awakening episodes which the doctor said were night terrors. At the time, they believed they were normal and that she would grow out of it. But, I knew that something wasn’t right with my baby. Tests were done and the doctors told me that Gabriella was having seizures! SEIZURES?? I felt like my heart was ripped from my chest! Gabriella was diagnosed with Intractable Epilepsy. This means that her seizures cannot be controlled. My heart aches every day having to watch Gabriella go through this. As her mother, I feel helpless knowing there’s nothing I can do to help her while she’s trying to fight through the seizures. They say God will not give us more then we can handle. Because God has given me the strength, I WILL continue to fight for Gabriella and other children like my daughter. That’s why I’ve started Team Gabriella with family and friends to walk in the 1st Annual Into the Light Walk for Epilepsy Awareness on Saturday, November 10th. You can join us or make a donation to support Gabriella by visiting www.epilepsyintothelight.org.
Q&A with Patricia McGoldrick, NP, MPA, MSN
NEXT UP: Our 1st Community Spotlight featuring Team Gabriella & The Epilepsy Road Warriors
The team at EFMNY would like to thank you for your questions! After each post, we’ll post answers from our experts to the most frequently asked questions we receive. Please note that these Q&A post, like our provider articles, should not be taken as medical advice. Each patient is unique. For medical advice regarding your specific condition, please consult your doctor.
Q&A with Patricia McGoldrick, NP, MPA, MSN:
1. I just found out that one of the medications I’ve taken for years is available in generic form. If it’s only one of the two medications I take, is there less risk in trying the generic?
This is difficult to answer without knowing which medications you are taking. Some of the medications in generic form are made by the same companies that make the brand name medications and so are consistent. The answer depends on the medications, the doses, how long you have been seizure free and a host of other issues. Please ask your provider, as he or she knows you best!
2. My daughter had surgery earlier this year. We were hoping that she would be medication free. However, she is still on meds. Is this typical for kids who have had epilepsy surgery?
The type of surgery, the medications, the length of time after the surgery and the cause of the epilepsy must all be taken into consideration, as well as the EEG findings and the post-operative MRI findings. Typically, medications are considered for some period of time after the surgery. Again, this is a great question for your provider! (more…)



