I Can Spell Electroencephalogram (EEG)
Recently, my neurologist ordered an EEG test for my epilepsy. EEG stands for electroencephalogram. An EEG records the electrical activity in your brain and it helps doctors detect abnormal electrical activity of the brain. Most types of EEG tests are considered relatively painless. However, like any medical test, from scheduling to prepping for the test, an EEG can always include some inconveniences and annoyances. Anyone who has ever had to remove EEG glue from their hair, understands why I call an EEG “relatively” painless.
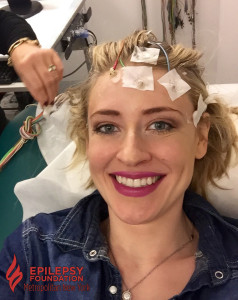
I had my first EEG test shortly after I was originally diagnosed with epilepsy when I was six years old. When my parents told me I had to undergo a new test related to my epilepsy, my first question was: “Are there any needles involved?” Luckily, my parents reassured me I would not be receiving a shot, getting an I.V. drip, or giving any blood. Plus, since my doctor prescribed me a sleep deprived EEG, the test prep required me to stay up late, preferably all night. Also, I got to miss a day of school, which was pretty cool! The next morning, my mother took me to my neurologist’s EEG lab. I was placed on a hospital bed and the technician glued electrodes to my head. After an hour of the technician asking me to breathe deeply and blink my eyes, they let me fall asleep. After I woke up, my electrodes were being removed from my head, and I returned home to go to bed. After several sleep deprived EEGs, I realized my mom also had to stay awake all night with me and miss work the next day. While I got to fall asleep for four hours during my EEG, my mom remained awake speaking with the technician or doctor. Now, as an adult, I understand how much an epilepsy diagnosis affects the entire family, from diagnosis to treatment.
In my twenties, I underwent a medication change because I began having a lot of seizures, again. My neurologist prescribed me several 72 hour ambulatory EEGs. For three days, I had a head full of glued-on electrodes. The electrodes were connected to wires, and the wires were connected to a small box recording the results. I could go anywhere, as long as I was still connected to my EEG box and electrodes. At work, I hid my electrode-covered head with a stylish beanie or scarf, allowing me to feel “normal.” Unfortunately, by the end of the first 48 hours, my head was itching like crazy. There was no beanie or scarf to alleviate my itchy head without removing the electrodes; but if these were to fall off, the EEG may have to be repeated! Finally, after the 72 hours, I would return to my neurologist’s office to have the electrodes removed.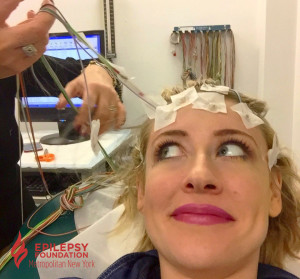
After any EEG, the inevitable issue of how to remove EEG glue arises. During this period of my life, I was not connected with the Epilepsy Foundation of Metropolitan New York, so I did not know the Epilepsy Foundation’s magic trick for removing EEG glue:
· Add 5 to 7 crushed aspirin to half a cup of hot water to dissolve. Then, add 2 good size squirts of shampoo, 4 tablespoons witch hazel or seabreeze, and mix well together. Massage the mixture through wet hair and let it sit for about 15 to 20 minutes. Finally, begin to comb through your hair after an allotted time has passed. Rinse and use shampoo and conditioner as usual.
I have never had to undergo a video-telemetry EEG test, which requires a patient to spend days in a hospital wearing an ambulatory EEG box, while being recorded by a video camera. Additionally, during a video-telemetry EEG test, epilepsy medications may be reduced or withdrawn, to increase the chances that you will have a seizure that can be recorded. So, while there are rarely needles involved, I would not dare to categorize all EEGs as “painless.”
 My recent standard EEG lasted for one hour and took place at my doctor’s office. It was the easiest EEG I had ever experienced. But, like epilepsy, even the types of EEG tests can vary. Like any medical procedure, it is important to stay informed and well prepared for an EEG test. The information an EEG test provides is essential for doctors treating epilepsy. Thankfully, this past EEG was totally painless because I finally knew how to remove EEG glue from my hair!
My recent standard EEG lasted for one hour and took place at my doctor’s office. It was the easiest EEG I had ever experienced. But, like epilepsy, even the types of EEG tests can vary. Like any medical procedure, it is important to stay informed and well prepared for an EEG test. The information an EEG test provides is essential for doctors treating epilepsy. Thankfully, this past EEG was totally painless because I finally knew how to remove EEG glue from my hair!
My Epilepsy Story
I recall the day I had my first seizure very well. I was walking into the room where a school-wide mass was taking place when suddenly, as the music began, I became very anxious. Everything seemed to be in slow motion – even the music slowed down and I started to shake. I did everything I could to continue standing but the pain was too great. I slowly dropped to the floor. At one point, I thought I was dying (I thought this was the end). I woke up to the comforting smiles of my middle school’s vice-principal and nurse. My body was physically drained. They told me I had a seizure.
What was a seizure? For someone who had no bad medical history, why me? The shock of the diagnosis of Epilepsy was a bit overwhelming in and of itself, but then I had to learn all about it. All of it seemed so surreal. Over the next two years I went through countless seizure-drug combinations, some of which drastically changed my mood. At one point, brain surgery was discussed.
I was already struggling with anxiety but the diagnosis only made things worse. I constantly would wonder “When would my next seizure happen?” I was terrified. Seizures didn’t just affect me physically, they affected me emotionally and socially. During Middle School, I was nervous when I wasn’t around an adult. Also, I felt other students didn’t really understand me, some were even scared to have me around. There was always a sense of guilt and that I just caused ‘extra work’ for everyone; often I just wanted to disappear.

In the 9th grade I starting to become very socially withdrawn and didn’t feel accepted. I began to spend more time composing and engineering music, whether it be in the hospital, my room or a local studio. I caught a break and started working with major songwriters and recording artists, while continuing school. Throughout high school, I only had a few people I could confide in. There aren’t a lot of people who will understand those daily struggles. Most never saw the tears or the endless nights in the hospital.
When I graduated June 2014, my seizures were finally controlled by medication. I recently started college, focusing on graphic design, while continuing on music collaborations. I consider myself extremely blessed to have had great support from family, teachers, doctors and school nurses.
My dream is to create a career in the arts, one that will help inspire other struggling artists to persevere and push beyond the seemingly hopeless circumstances they sometimes face in life.
Growing-Up With Epilepsy and Learning to Speak Out at School and in the Workplace
Epilepsy is difficult to explain, describe and understand. People can only “see” epilepsy when someone is having a seizure. For many people with epilepsy, seizures are unpredictable and, sometimes, undetectable to others. In my case, most of my seizures have been tonic-clonic, or grand-mal, seizures. Tonic-clonic seizures are hard to miss. However, unless I’m having a violent seizure, no one would know I have epilepsy, until I open my mouth. I talk a lot about my epilepsy. Communicating with others about my epilepsy keeps me safe and helps me take control. As a person with epilepsy, I force myself to keep an open and honest dialogue with all of my medical professionals, my peers and my work colleagues.
I was five when first diagnosed with epilepsy after having absence, or petite-mal, seizures. At the time, I did not mind the epilepsy diagnosis because my seizures were not visible to me. Then, I learned I had to take monthly blood tests…with needles! I dreaded blood tests and I did not go softly or quietly into the pathology lab. It was stressful for me; every time I knew I was getting another blood test I would start crying and screaming. Finally, a lab technician took a moment to speak with me. I expressed to him my fear of needles. He offered to take my blood with a smaller needle he called a “butterfly,” and it would not hurt as much. I agreed to cooperate calmly. One conversation changed my entire attitude towards blood tests and my behavior at the lab. The recommended “butterfly” needle might have reduced the physical pain, but in hindsight, it was the technician who calmed me down by communicating with me and addressing my fears. At the age of six, I found power and control by openly communicating with all of my doctors and medical professionals.
 My first tonic-clonic, or grand-mal, seizure happened when I was in junior high school. Epilepsy is a difficult thing to openly discuss, especially during those awkward adolescent years. After many in-class seizures, I realized it was difficult and scary for my peers to witness one of my seizures. So, I took responsibility, and talked openly about my epilepsy. There were some students who used my epilepsy as a way to bully and tease me. A few kids called me “seizure girl.” I endured other unpleasant instances of bullying targeted at my epilepsy. Fortunately, I did not care about the opinion of those who bullied me. They did not want to communicate; they wanted to attack.
My first tonic-clonic, or grand-mal, seizure happened when I was in junior high school. Epilepsy is a difficult thing to openly discuss, especially during those awkward adolescent years. After many in-class seizures, I realized it was difficult and scary for my peers to witness one of my seizures. So, I took responsibility, and talked openly about my epilepsy. There were some students who used my epilepsy as a way to bully and tease me. A few kids called me “seizure girl.” I endured other unpleasant instances of bullying targeted at my epilepsy. Fortunately, I did not care about the opinion of those who bullied me. They did not want to communicate; they wanted to attack.
My seizures were controlled during high school. Although my epilepsy wasn’t visible, my parents and doctors strongly encouraged me to continue to disclose my condition. I often had to explain to friends I did not go to concerts because most concerts have strobe lights, a trigger for seizures. After I turned sixteen, I knew communicating my health issues was a legal and ethical responsibility as a licensed driver. I was becoming an adult and I needed to learn to talk about my epilepsy independently from my parents and pediatric doctors.
In my early twenties, I started having seizures, again. I was new to the New York City workforce and I knew little about how to talk about my disorder in the workplace. I never knew when to disclose my condition or who to disclose my condition to. As an adult, communicating about epilepsy, or any disability, in the workplace can be a grey area. I did not know if I should mention my epilepsy before or after I interviewed for a new job. Most companies do not encourage people to ask others their health issues, due to privacy laws. At twenty-seven, my epilepsy was uncontrollable and I needed to change my medications (AEDs). At the time, I was having seizures at work and felt devalued as an employee, even though I had a better attendance record than many of my colleagues. In fact, I had a superior criticize me via email for not drinking and socializing at an after-hours company event. I realized the people I was working with did not want to communicate openly and honestly about my epilepsy. Like the bullies in junior high, I stopped communicating with them. Instead, I communicated with my doctors and a lawyer. I filed for the Family Medical Leave Act. This provided me some short-term job protection. It also gave me a chance to stand up for myself against employers and colleagues who tried to exploit my condition as a weakness. My epilepsy is a neurological disorder, not a weakness.
I am still figuring out the best way to live and work openly as a person living with epilepsy. Luckily, I have connected with the Epilepsy Foundation of Metropolitan New York to learn more. The EFMNY provides tools to help facilitate communication and understanding about epilepsy. It provides New York City’s only specialized job development and vocational services program for people with epilepsy. Few people understand epilepsy and epilepsy’s far-reaching effects on a person’s life. So, as a person with epilepsy, I find it easier to tell others about my condition. People are sometimes afraid to ask questions about a disability or condition out of fear of being offensive or sounding stupid. So, I try to beat them to the punch and talk about my epilepsy first. It is important to help educate, explain and remove the stigma. I will never have complete control over my epilepsy, but I have complete control over my conversations about epilepsy.
-Alexandra DeBourcy, Mrs. Gotham City
Me and My Epilepsy – Mrs. Gotham City
My name is Alexandra DeBourcy and my epilepsy is a part of my life, my history and my future.
I was diagnosed with epilepsy at the age of five, when my parents noticed I was having “head tics.” Shortly after starting my epilepsy medication, I stopped experiencing myoclonic tics. As a 5 year-old, I did not understand the full extent of my diagnosis, but I recognized a change in my lifestyle. At that very young age, I had to swallow non-chewable prescription medication, undergo many boring diagnostic tests and take monthly blood tests. The blood tests were the worst. Even at five, I knew my epilepsy diagnosis was changing my life.
Despite years of living seizure-free, one day during class when I was in the 7th grade, I had my first ever grand-mal seizure. When I awoke, I was still in school, surrounded by working paramedics, as well as teachers and school administrators whose faces were filled with panic and fear. It took me a while to understand I had just had a seizure. At the time, I could only think about how my peers, who also witnessed my seizure, would judge me. Prior to returning to school, I called some of the students in class. It was easier to explain my epilepsy on a one-on-one basis. It helped. I don’t know if my phone calls helped any of my classmates, but it I do know it helped me. It gave me strength to face my schoolmates. I had more grand mal seizures in school during my adolescence, but I continued to open up and discuss my epilepsy with classmates and adults.
Luckily, I remained seizure free during high school and most of college, but my epilepsy was still a part of me. My parents and doctors reinforced the need for me to communicate my disorder to my friends, teachers and professors. No matter how long I went without a seizure, I had a different lifestyle than my peers. I was approaching the age where my actions, especially as a driver, had a greater effect on the lives of others. So, I continued to use communication, and levity, to introduce my epilepsy to other people.
After graduating from Syracuse University, I started having grand-mal seizures, again. This added additional considerations, as I was about to begin my career search. My epilepsy stabilized, and I moved to New York City. I loved New York City, and it had a public transportation system I could depend on. I was able to find work at an ad agency with an insurance plan. Since I had been denied a private insurance due to my pre-existing condition.
Unfortunately, I continued to experience seizures through out my twenties. I also experienced the Great Recession, the election of our first Black President, and falling in love with my husband. Eventually, my doctors and I decided to change medications. I had seizures at work. Some of my colleagues were empathetic; others were not. I sometimes felt stigmatized in my work environment. Due to privacy laws, it was hard for employers and colleagues to talk openly with me about my epilepsy.
Eventually, I left advertising. It was not the best career environment for my epilepsy. I decided to change careers and become a gemologist. My change in careers has allowed me to work in an environment more suitable for my epilepsy. I also work very happily with diamonds, gems and beautiful jewelry. It also has provided me with more time to devote to helping others with epilepsy. I now have the chance to represent the Epilepsy Foundation of Metropolitan New York as Mrs. Gotham City in the upcoming Mrs. New York America pageant.
I have had to accommodate my epilepsy throughout my entire life and, many times, I have resented my epilepsy. However, the happiest times in my life occurred when I worked with my epilepsy without shame. It is embarrassing to have a seizure in school or at work. It is awkward to tell peers about a personal neurological disorder. Furthermore, it is difficult to disguise EEG electrodes for three days straight. So, as an epileptic, I know I can empower myself by starting the conversation on my epilepsy. I want to continue and expand the conversation with others living and affected by epilepsy. It is the best way I know to keep myself safe and happy. We need to discuss new treatments, gather community support and take the stigma away from epilepsy.
Epilepsy and Driving
Dear EpilepsyNYC Community,
Because of my epilepsy, I have never driven a car.
When I was around 17 years old, like many of my friends at that age, I was saving my allowance with the hopes of using the money to buy a car. I remember saying to my parents “When I drive, I’ll get in my car and go everywhere.” Driving represented freedom.
Around this time, the medication I had been on since I was diagnosed (age 11), wasn’t working like it once did. My doctor at the time, decided to put me on a new medication without taking me off the medication that was no longer working. As a result I got really dizzy at school and fell down the stairs; I was over medicated. I ended up missing school for a week, and needless to say, changed doctors after that.
It was my new doctor who broke the news: I wouldn’t be able to drive. I remember taking my car money out of the tin can it was in, feeling crushed. My dream of driving was gone. Even when I think back on it, after everything that has happened since then, I still get a little sad.
 I’ve met people with epilepsy who drive, but epilepsy is different for every person and every state has different rules about driving with epilepsy. Here in New York you have to be seizure free for a year and your doctor has to approve. Unfortunately, I have never spent a full year seizure free. And though there are bigger problems I have with epilepsy, I still wish I could drive.
I’ve met people with epilepsy who drive, but epilepsy is different for every person and every state has different rules about driving with epilepsy. Here in New York you have to be seizure free for a year and your doctor has to approve. Unfortunately, I have never spent a full year seizure free. And though there are bigger problems I have with epilepsy, I still wish I could drive.
Many of my friends tell me, “Don’t worry Kate, driving is overrated,” and I can understand their perspective, between the gas prices and traffic jams… But maybe they are simply trying to make me feel better. I can’t believe driving is overrated, and perhaps that is because I’ve never driven; I always have to be asking for a ride to go anywhere, when for almost everyone else, it seems as easy as just hopping into a car.
Like many of us do in New York, I complain about public transportation and taxi drivers, but I know that it could be worse. I am lucky to live in a city where I can get around easily. I can walk, take the bus, train or take a cab to get where I need to go. I hear about people living in places where it takes them 30 minutes just to get to the grocery store. I know it would be much more difficult for me if I lived somewhere where it was hard to commute. I am grateful, but some days are easier than other days. Some days I don’t feel comfortable taking public transportation or cabs.
Around 8 years ago, when I was on my way to school, I had a seizure on the bus. And 3 years ago, I had a seizure in a cab. I can only assume the cab driver didn’t know what to do or got scared, because he drove away and left me on the street, only a few blocks away from where I started.
It is frustrating when epilepsy controls your life, and ones ability to drive is certainly something epilepsy controls. It prevents you from freely doing what you need to do and going where you want to go.
I do hope one day I will be able to drive, but I also don’t want to put myself or anyone else on the road in danger. On the news, my parents and I heard that they are making cars that drive themselves. Maybe one day I can use one of those?
If one day I can drive that will be one less thing that my epilepsy controls.
My Life With Epilepsy
Dear EpilepsyNYC Community,
I am Kate Spratt. I am 28 years old, and I have epilepsy.
When I was six years old, I had my first seizure: on Christmas Eve, I was looking at the twinkling lights on our Christmas tree and my Grandma was talking to me but I wasn’t responding, I just kept looking at the lights.
However, I don’t remember this. All I remember is waking up in the hospital and being very confused. Worried that I was going to miss out on Christmas, I spent that night in the hospital having multiple tests and a spinal tap done. After that, for the next five years of my life, I was seizure free.
Then suddenly, when I was eleven, I had three grand-mal seizures and I was put on medication. During my pre-teen and teenage years, my seizures were under control (for the most part). I did have some “jerks,” but they didn’t affect me enough to debilitate me. I went to school, hung out with my friends, and participated in after school activities. I am grateful for that. I didn’t really talk about my epilepsy when I was a teenager, only a few of my close friends knew. Looking back, I think I didn’t tell people because I wasn’t sure how they would react.
Then, when I was around sixteen, I was in class one day, about to take a test, and I had a seizure. Next thing I knew, I was on my side, on the floor, and the ambulance was there. Luckily, my teacher at the time, used to work with children who had epilepsy and knew what to do when a student had a seizure. I had never had a seizure in school before. I was very tired (as I usually am after a seizure), but mostly very embarrassed. I swore I wouldn’t go back to school.
That night, the teacher called my house and spoke with my mom. She wanted to see how I was doing, and knowing I was probably embarrassed, also wanted me to know that everyone was very concerned about me. When my mom told me, I was relieved, but still kind of nervous of how people would react. Upon my return to school, no one said anything. When one girl shyly asked if I was feeling better I realized people were concerned. It was time to tell my friends, all my friends. Because seizures can happen, anywhere at any time, and people should know what to do.
Opening up about my epilepsy made my classmates comfortable enough to open up to me. I realized that a lot of people had family-members who had it too, while others, who were not familiar with epilepsy, wanted to know more. I knew then it wasn’t something to be embarrassed about; it was just a part of me. I think of it like this: some people have allergies, some people have asthma, and some people have epilepsy.
I proceeded to go to college and graduated with a Bachelor of Science in Secondary Education, with a 3.15 GPA and in four years. I did miss days sometimes because I had seizures and couldn’t go to school. I once even fell down the stairs on campus because I just kept walking and couldn’t stop. Graduating college was a huge accomplishment for me, because of how challenging it was at times. I couldn’t pull “all-nighters” like other students, and the workload could be quite stressful.
After graduating from college, I found a job that I loved at an after school program. On May 18, 2009, while I was taking a shower to get ready for work, I reached over, simply to adjust the water temperature slightly, and had a seizure, which caused me to accidentally turn the hot water on all the way and fall down. I don’t know how long I was under the scalding hot water and when I re-gained consciousness I didn’t even realize I was burnt; it was like I was in a fog. Twenty percent of my body was scalded and I had third degree burns. My whole back, my left arm and my thumb were burnt. I was in the hospital for five weeks. They said if I had passed out face forward I would have died. I had three skin grafts, I couldn’t walk, I couldn’t bend down, and I didn’t have range of motion in my arm for months. I had to wear compression garments for a year and do months and months of physical therapy in the hospital and everyday at home with my dad.
Ever since 2009 my epilepsy has gotten worse; the doctors don’t know why this is or why I even have epilepsy. No one in my family has ever had it, I never ran fevers as a child, or had any head injuries. I’ve been hospitalized numerous times and endured all sorts of different side effects brought on by my medications. I’ve been on so many different medications it feels like I’ve been on every AED out there.
I have my ups and downs with my epilepsy. I try to stay strong or say that I’m a medical mystery, since no one knows why or how my epilepsy has gotten worse. It’s always great when you take a few steps forward but such a defeat when you then take those steps back. Because of everything that has happened, especially in the past few years, people don’t understand how I’m an optimist. When it comes down to it, it would probably be easier to be a pessimist, but it’s important to appreciate the good things in your life, like your family and friends, the moments when you’re not having seizures, and most of all, the fact that I’ll never give up hope for that one day when I’ll stop being a medical mystery.
